Every 40 seconds, someone in the United States has a heart attack. In India, cardiovascular disease claims nearly 2.8 million lives every year — more than any other cause. Globally, the World Health Organization reports that heart disease is the number one killer of both men and women worldwide, accounting for 17.9 million deaths annually.
Here is the hardest truth: many of those deaths were preventable. Not because treatment wasn’t available — but because the person having the heart attack, or the people around them, did not recognise what was happening in time.
The movies have taught us to expect a dramatic, unmistakable event — a sudden clutching of the chest, a collapse to the floor. In reality, a heart attack can feel like indigestion. Like a sore shoulder. Like unusual tiredness after a normal day. It can happen without any chest pain at all. It can come on gradually, over hours or even days, as quiet, easy-to-dismiss warning signals that the body is sending before the crisis becomes irreversible.
This guide exists because knowing the warning signs is the single most powerful thing you can do to survive a heart attack — and to help someone else survive one. We will cover every symptom, the critical differences between how heart attacks present in men versus women, the dangerous reality of silent heart attacks, the risk factors that put you at higher risk, the immediate actions that can save a life in the first minutes, and the long-term steps that can prevent a heart attack from ever happening.
Read this. Share it. Knowing this information is not dramatic — it is responsible.

📋 Table of Contents
- What Is a Heart Attack? Understanding the Basics
- The 10 Classic Heart Attack Warning Signs
- Heart Attack Warning Signs in Women: The Critical Differences
- Heart Attack Warning Signs in Men
- The Silent Heart Attack: When There Are No Warning Signs
- Warning Signs That Can Appear Days or Weeks Before
- Immediate Actions to Take — Every Second Counts
- Risk Factors: Who Is Most Vulnerable?
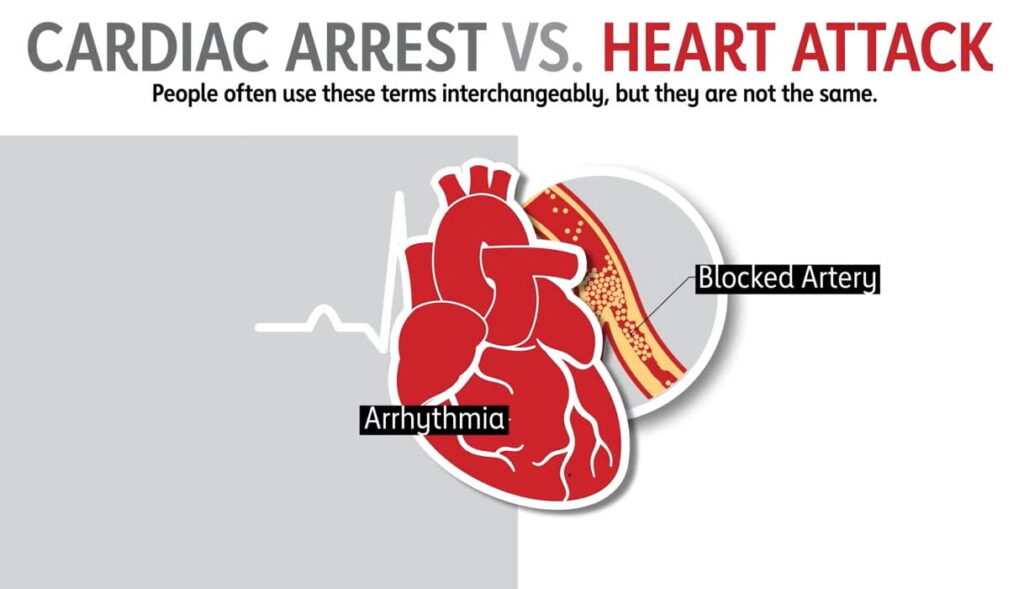
- Heart Attack vs. Cardiac Arrest: Understanding the Difference
- How to Prevent a Heart Attack: Science-Backed Steps
- Life After a Heart Attack: Recovery and What to Expect
- Frequently Asked Questions
What Is a Heart Attack? Understanding the Basics
A heart attack, medically known as a myocardial infarction (MI), occurs when blood flow to a part of the heart muscle is severely reduced or completely blocked. The word itself is instructive: “myo” means muscle, “cardial” refers to the heart, and “infarction” means the death of tissue due to lack of blood supply.
The heart is a muscle. Like every other muscle in the body, it needs a constant supply of oxygen-rich blood to function. That blood is delivered through the coronary arteries — the blood vessels that wrap around the outside of the heart. When one or more of these arteries becomes blocked, the section of heart muscle it supplies begins to die. The longer the blockage continues, the more tissue is permanently damaged.
How Does a Blockage Form?
Most heart attacks are caused by atherosclerosis — a condition in which fatty deposits (called plaque) build up inside the walls of the coronary arteries over time. This plaque is made up of cholesterol, fat, calcium, and other substances from the blood.
Over years or decades, this plaque hardens and narrows the artery, restricting blood flow. A heart attack typically occurs when a piece of plaque ruptures, causing a blood clot to form suddenly at that site. This clot can rapidly block the artery entirely, cutting off blood supply to the heart muscle within minutes.
This is why time is the most critical factor in a heart attack. Every minute that passes without restored blood flow means more heart muscle dying permanently. Treatments like percutaneous coronary intervention (PCI) — where a blocked artery is physically opened — work best within the first 60–90 minutes. The phrase used by cardiologists is: “Time is muscle.”
The 10 Classic Heart Attack Warning Signs You Must Know
The following warning signs are the ones that cardiology organisations around the world — including the American Heart Association, Mayo Clinic, and the World Health Organization — consistently identify as the primary signals of a heart attack in progress. Not every person will experience all of them. Some people experience only one or two. The critical rule is: if you suspect a heart attack, do not wait for more symptoms to confirm it. Act immediately.
1Chest Pain, Pressure, or Discomfort
This is the most well-known and most common heart attack warning sign — but it is frequently misunderstood. Many people expect crushing, unbearable pain that is impossible to ignore. In reality, chest discomfort during a heart attack is often described as:
- A feeling of pressure or squeezing in the centre of the chest — like a heavy weight pressing down
- Tightness or fullness, as if the chest is being gripped from the inside
- A dull, persistent ache or burning sensation
- Discomfort that comes and goes over several minutes rather than being constant
The discomfort is typically located in the centre or left side of the chest and usually lasts more than a few minutes. Crucially, it may go away and return. Never dismiss chest discomfort that is new, unusual, or persists — even if it does not feel like what you imagine “heart attack pain” should feel like.
2Shortness of Breath
Sudden difficulty breathing — feeling unable to get enough air, becoming breathless with minimal exertion, or waking up gasping for air — can be a serious heart attack warning sign. It may occur with or without chest discomfort.
When the heart is unable to pump blood effectively (because a coronary artery is blocked), fluid can back up into the lungs, causing breathlessness. This symptom should never be attributed to anxiety or overexertion without proper evaluation, especially if it is new or sudden.
3Pain That Radiates to the Arm, Shoulder, Back, Neck, or Jaw
One of the most diagnostically important — and most frequently missed — heart attack warning signs is pain or discomfort that travels beyond the chest. The heart shares nerve pathways with other areas of the upper body, which means the brain can interpret heart pain as originating somewhere else entirely. This is called referred pain.
Common radiation patterns include pain down the left arm (the classic Hollywood version, but it also happens in the right arm), pain in one or both shoulders, pain in the upper back or between the shoulder blades, pain in the jaw, neck, or throat, and an unusual ache in the upper abdomen that may be confused with a stomach problem. Pain in the jaw in particular — especially in women — is frequently dismissed as dental pain. It is not. If jaw pain arrives alongside any other unusual symptoms, treat it as a potential cardiac emergency.
4Cold Sweats (Diaphoresis)
Breaking out in a sudden, unexplained cold sweat — particularly when you are not physically exerting yourself and the environment is not hot — is a significant heart attack warning sign. The medical term for this is diaphoresis, and it happens because the body’s sympathetic nervous system is activated during a cardiac event.
The sweating often feels different from normal perspiration — it is clammy, comes on suddenly, and is typically accompanied by pallor (paleness) or a grey tinge to the skin. If you or someone near you suddenly looks pale and sweaty without obvious cause, take it seriously.
5Nausea, Vomiting, or Indigestion-Like Discomfort
This is one of the most dangerous heart attack warning signs — dangerous because it is so easy to attribute to something harmless. Nausea, vomiting, or a sensation that feels exactly like indigestion or heartburn can be the primary symptom of a heart attack, particularly in women.
The proximity of the heart to the stomach, and shared nerve supply, means that the brain can interpret cardiac pain as digestive discomfort. According to Mayo Clinic, many women who have heart attacks report experiencing what felt like stomach upset, heartburn, or flu-like nausea in the hours before the event. If indigestion-like symptoms appear suddenly alongside any other unusual feeling in the chest, jaw, back, or arms — call emergency services immediately.
6Lightheadedness or Dizziness
A sudden feeling of dizziness, faintness, or the sensation that you are about to pass out can occur during a heart attack. When the heart is not pumping effectively, blood pressure can drop rapidly, reducing blood flow to the brain and causing lightheadedness.
This symptom alone may have several non-cardiac explanations, but when it occurs alongside chest discomfort, shortness of breath, or arm/jaw pain, it becomes a significant warning sign. Do not sit or lie down and wait for it to pass — call emergency services immediately.
7Unusual or Extreme Fatigue
Profound, unexplained exhaustion — the kind that makes it feel difficult to carry out normal daily activities, or fatigue that persists even after rest — is one of the most commonly reported heart attack warning signs, particularly in women. It can appear days or even weeks before a full cardiac event.
According to research cited by the American Heart Association, unusual fatigue is one of the most frequently reported warning signs among women who have had heart attacks. It is often described as feeling “more tired than I’ve ever felt,” even after a full night’s sleep. If this kind of fatigue appears with no clear explanation, especially in someone with risk factors, it should prompt a medical evaluation.
8Heart Palpitations or Irregular Heartbeat
A sense that the heart is racing, fluttering, pounding unusually hard, or skipping beats can be a heart attack warning sign — though palpitations have many possible causes that are non-cardiac. During a heart attack, electrical disturbances in the damaged heart muscle can cause abnormal heart rhythms.
When palpitations occur alongside other warning signs — chest discomfort, breathlessness, sweating, or pain in the arm or jaw — they become much more significant. Do not wait to “see if they pass.” Seek medical attention immediately.
9Anxiety or a Sense of Impending Doom
This is perhaps the least-discussed but one of the most powerful heart attack warning signs. Many heart attack survivors have described an overwhelming feeling of anxiety, fear, or a profound sense that “something is very wrong” — often without being able to identify a specific physical symptom that explains it.
This is not psychological weakness. It is a physiological response — the body’s fight-or-flight system being activated by the cardiac emergency it is experiencing. If you or someone you are with suddenly experiences severe, unexplained anxiety, especially in the context of other unusual physical sensations, treat it as a warning sign.
10Swelling in the Legs, Ankles, or Feet
While this is more commonly associated with heart failure than a sudden heart attack, persistent swelling (called oedema) in the lower extremities can be a sign that the heart is struggling to pump blood efficiently. Fluid backs up in the body’s tissues, particularly in the legs and ankles due to gravity.
If you notice unusual swelling in your legs or ankles — especially if accompanied by shortness of breath, unusual fatigue, or a persistent cough — consult a healthcare provider promptly. This can indicate deteriorating heart function that raises the risk of a cardiac event.
You do not need to have all of these symptoms to be having a heart attack. You do not need severe symptoms. The more warning signs present together, the more likely it is to be a heart attack — but even one unexplained symptom that is new and unusual deserves immediate medical attention. According to the American Heart Association: “Even if you’re not sure it’s a heart attack, call 911 or your country’s emergency services immediately.”
Heart Attack Warning Signs in Women: The Critical Differences
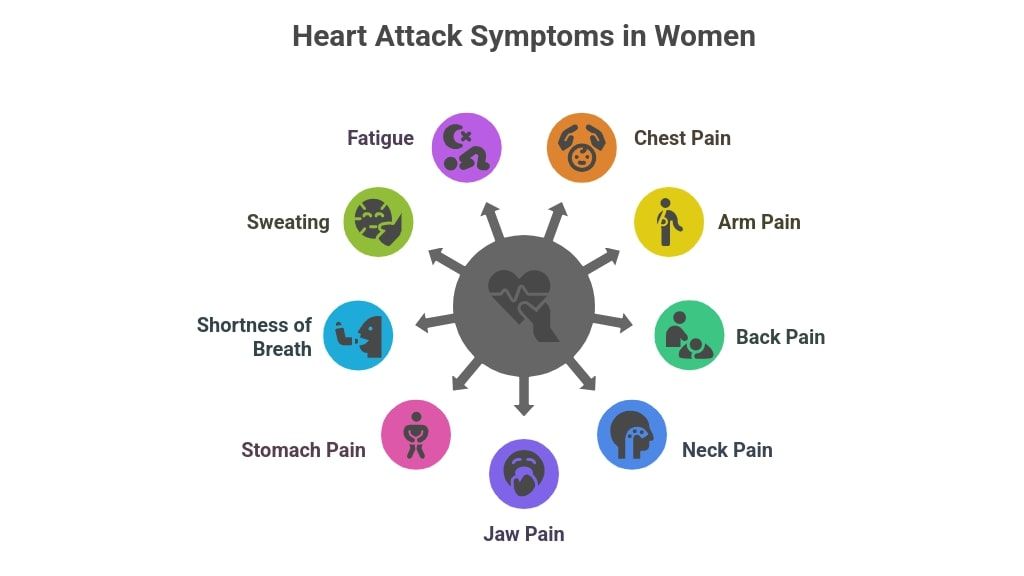
One of the most important and underappreciated medical realities of the past two decades is this: women’s heart attacks often look and feel different from men’s heart attacks. This difference has been responsible for a significant number of preventable deaths, because women are more likely to dismiss their symptoms as stress, anxiety, indigestion, or the flu — and because healthcare providers have historically been less likely to recognise cardiac events in women who present without classic chest pain.
“Even though heart disease is the No. 1 killer of women in the U.S., women often chalk up the symptoms to less life-threatening conditions such as acid reflux, the flu, or normal aging.”— American Heart Association, Heart Attack Symptoms in Women
Why Women’s Heart Attack Symptoms Differ
Women are more likely to have what are called non-obstructive coronary artery disease events — heart attacks that occur not from a single massive plaque rupture in a large artery, but from smaller blockages, coronary spasms, or microvascular disease affecting the tiny blood vessels of the heart. These mechanisms often produce symptoms that are more diffuse and less classically dramatic than the “Hollywood heart attack.”
Hormonal differences (particularly the protective effect of oestrogen before menopause, which is lost afterward), different distributions of coronary artery anatomy, and neurological differences in pain perception all contribute to the different symptom profile that women experience.
Heart Attack Warning Signs More Common in Women
According to both the Mayo Clinic and the American Heart Association, the following heart attack warning signs are significantly more common in women than men:
- Unusual fatigue — often extreme and present for days or weeks before the cardiac event
- Nausea, vomiting, or indigestion — frequently mistaken for stomach illness or acid reflux
- Jaw, neck, or upper back pain — often present without any chest pain at all
- Shortness of breath without chest pain — breathlessness on minimal exertion or at rest
- Sleep disturbances — unusual difficulty sleeping in the weeks preceding a heart attack
- Anxiety and a sense of unease — often attributed to stress rather than a cardiac event
- Pain in one or both shoulders — sometimes without any sensation in the chest
- Dizziness or lightheadedness
- Cold or clammy sweat
Women-Specific Risk Factors
In addition to the general risk factors for heart disease, women face unique biological risks that are not present in men:
- Menopause — The drop in oestrogen after menopause increases the risk of coronary artery disease and small vessel heart disease significantly
- Polycystic Ovary Syndrome (PCOS) — Associated with increased cardiovascular risk
- Gestational diabetes or preeclampsia — Complications during pregnancy that elevate long-term heart disease risk
- Oral contraceptive use combined with smoking — Significantly increases the risk of blood clots and heart attack
- Autoimmune conditions — Lupus, rheumatoid arthritis, and scleroderma raise cardiovascular risk, and these conditions affect women more than men
- Diabetes in women — Carries a higher relative risk for heart attack compared to diabetes in men
Heart Attack Warning Signs in Men
While men experience the full range of heart attack warning signs described in the classic list above, their presentation is statistically more likely to include the “textbook” symptoms — specifically, the crushing or squeezing chest pain that radiates down the left arm.
However, the very familiarity of this presentation can be its own danger. Men who are experiencing a heart attack sometimes minimise their symptoms, rationalise them as indigestion or muscle strain, or delay calling emergency services because they are “not sure” the symptoms are serious enough. The number one mistake people make during a heart attack is waiting too long to call for help.
Symptoms Men Are More Likely to Experience
- Classic crushing, squeezing, or heavy chest pain or pressure
- Left arm pain or numbness
- Profuse sweating alongside chest discomfort
- Sudden loss of consciousness or near-fainting
- Heart palpitations or arrhythmia
The Silent Heart Attack: When There Are No Warning Signs
Perhaps the most alarming reality in cardiac medicine is this: between 50% and 80% of all heart attacks may be “silent” — occurring with minimal symptoms, symptoms that are too vague to identify as cardiac, or no symptoms at all. Many people discover they have had a silent heart attack only weeks or months later, when an electrocardiogram (ECG) reveals evidence of old heart muscle damage.
According to Cleveland Clinic, a silent myocardial infarction (SMI) causes the same type of permanent heart muscle damage as a classic heart attack — but the person having it may attribute any symptoms they do feel to something entirely different:
- A pulled muscle in the chest or back
- Indigestion or heartburn
- The flu or general illness
- A bout of unusual fatigue
- Jaw or tooth pain
Who Is at Greatest Risk of a Silent Heart Attack?
Silent heart attacks are more common in people with diabetes, because diabetes can damage the nerves responsible for transmitting pain signals, reducing the ability to feel the classic chest pain of a heart attack. They are also more common in older adults and in women, particularly those over 60.
Because a silent heart attack is not recognised in real time, the person does not seek treatment. The heart muscle that dies during that event is never treated. If the person then has a second, more classic heart attack, they are starting from a position of already having sustained cardiac damage — which significantly worsens the prognosis. According to a study referenced by Asian Heart Institute, people who have had a silent heart attack have the same long-term mortality risk as those who had a recognised heart attack. But because they don’t know what happened, they are far less likely to be on preventive medication or making lifestyle changes.
Warning Signs That Can Appear Days or Weeks Before a Heart Attack
One of the most valuable and under-taught pieces of cardiac knowledge is that a heart attack often does not arrive without warning. The body frequently sends signals in the hours, days, and even weeks before a major cardiac event — signals that, if recognised, can prompt early intervention that prevents the heart attack from occurring at all or significantly reduces its severity.
The Pre-Attack Warning Window
The following symptoms, when new, persistent, and unexplained, can be early-warning signals that warrant immediate medical evaluation:
| Warning Sign | Why It Happens | Who Experiences It Most |
|---|---|---|
| Unusual fatigue, persistent for days | Heart working harder to compensate for reduced blood flow | More common in women (70% of female heart attack cases) |
| Recurring indigestion or stomach discomfort | Referred pain from reduced coronary blood flow | Women and people with diabetes |
| New shortness of breath during mild activity | Heart struggling to maintain adequate output | Both men and women, especially older adults |
| Chest tightness that comes and goes | Unstable angina — partial or temporary blockage | Men more commonly; also women |
| Sleep disturbances or waking gasping | Possible reduced oxygen delivery during sleep; anxiety | More common in women pre-heart attack |
| Swollen ankles or feet | Early heart failure — reduced cardiac pump efficiency | Both, especially people with existing heart disease |
| Unexplained anxiety or a “something is wrong” feeling | Sympathetic nervous system activation in response to cardiac stress | Both men and women |
Immediate Actions to Take — Every Second Counts
If you believe you or someone near you is experiencing a heart attack, the following actions can make the difference between life and death. Do not hesitate. Do not second-guess. Every minute of delay means more permanent heart muscle damage.
What NOT to Do During a Heart Attack
- ❌ Do not drive yourself to the hospital — you could lose consciousness at the wheel. Call an ambulance.
- ❌ Do not wait more than 5 minutes to see if symptoms improve before calling for help
- ❌ Do not eat or drink anything — the person may need emergency surgery
- ❌ Do not give someone aspirin if you don’t know whether they are allergic or if they are already on anticoagulant medication
- ❌ Do not leave the person alone while waiting for emergency services
- ❌ Do not let someone talk you out of calling for help — people having heart attacks often resist emergency help. Overrule them.
Risk Factors: Who Is Most Vulnerable to a Heart Attack?
Understanding who is at elevated risk is as important as recognising the warning signs — because risk factor management is the foundation of heart attack prevention. Many of the most significant risk factors for heart attack are modifiable — meaning they can be reduced or eliminated through lifestyle changes and medical management.
🩸 High Blood Pressure
Hypertension damages and stiffens artery walls, accelerating atherosclerosis and increasing the risk of plaque rupture. It is one of the most common — and most treatable — risk factors for heart attack.
🍔 High Cholesterol
Elevated LDL (“bad”) cholesterol is the primary driver of plaque build-up in the coronary arteries. Combined with low HDL (“good”) cholesterol, it significantly increases heart attack risk.
🚬 Smoking
Tobacco smoke damages the lining of blood vessels, promotes clot formation, reduces HDL cholesterol, and dramatically increases heart attack risk. Quitting smoking cuts cardiovascular risk by 50% within one year.
🍬 Diabetes
High blood glucose damages blood vessels and accelerates coronary artery disease. People with diabetes have a 2–4 times higher risk of dying from heart disease than people without diabetes.
⚖️ Obesity
Being overweight — particularly with central obesity (excess fat around the abdomen) — raises blood pressure, worsens cholesterol profiles, promotes insulin resistance, and elevates inflammatory markers linked to cardiac events.
🛋️ Physical Inactivity
A sedentary lifestyle independently doubles the risk of heart disease. Regular physical activity reduces blood pressure, improves cholesterol, lowers body weight, and improves heart muscle function.
👨👩👧 Family History
A first-degree relative (parent or sibling) who had a heart attack before age 55 (men) or 65 (women) significantly increases your risk. This is a non-modifiable risk factor — but it makes monitoring other risk factors even more critical.
😰 Chronic Stress
Prolonged psychological stress elevates cortisol and adrenaline, increases blood pressure, promotes unhealthy behaviours (poor diet, smoking, inactivity), and may directly contribute to coronary artery disease.
🍷 Excessive Alcohol
Heavy drinking raises blood pressure, contributes to obesity, and can cause direct damage to the heart muscle (cardiomyopathy). Moderate consumption (if any) is the only safe level from a cardiac perspective.
🎂 Age
Risk increases significantly with age — particularly after age 45 in men and after menopause in women. However, heart attacks can and do occur in young adults, including people in their 20s and 30s.
Heart Attack vs. Cardiac Arrest: Understanding the Vital Difference
These two terms are frequently confused — and in an emergency, the confusion can be fatal. They are not the same condition, they have different causes, and they require different responses.
| Feature | Heart Attack | Cardiac Arrest |
|---|---|---|
| What it is | A blocked coronary artery cuts blood supply to part of the heart muscle | The heart’s electrical system fails, causing the heart to stop beating entirely |
| Consciousness | Person is usually conscious and experiencing symptoms | Person loses consciousness immediately and has no pulse |
| Breathing | Usually still breathing (may be laboured) | No normal breathing |
| Connection | A heart attack can cause cardiac arrest | Can occur with or without a preceding heart attack |
| Immediate response | Call emergency services; keep calm; aspirin if appropriate | Begin CPR immediately; use AED if available; call emergency services |
| Window for survival | Best outcomes within 60–90 minutes of first symptom | Brain damage begins within 4–6 minutes; death within 10 minutes without CPR |
How to Prevent a Heart Attack: Science-Backed Steps
The good news at the centre of all this information is that the majority of heart attacks are preventable. According to the American Heart Association’s Life’s Essential 8 framework, addressing eight key health factors can dramatically reduce cardiovascular risk.
1. Know and Control Your Blood Pressure
High blood pressure is the single most important modifiable risk factor for heart attack and stroke. Most people with hypertension have no symptoms — which is why it is called the “silent killer.” Get your blood pressure checked regularly, understand your numbers (ideal: below 120/80 mmHg), and follow your doctor’s advice on management through diet, exercise, and if necessary, medication.
2. Manage Cholesterol Levels
Ask your doctor for a full lipid panel — this measures LDL (“bad”) cholesterol, HDL (“good”) cholesterol, and triglycerides. Keep saturated and trans fats low in your diet, increase soluble fibre (oats, legumes, vegetables), and maintain a healthy weight. If lifestyle measures are insufficient, statins or other cholesterol-lowering medications are highly effective.
3. Control Blood Sugar
Pre-diabetes and type 2 diabetes dramatically increase heart attack risk. Have your fasting blood glucose and HbA1c tested regularly, maintain a diet low in refined carbohydrates and added sugar, and engage in regular physical activity — which is one of the most effective ways to improve insulin sensitivity.
4. Exercise Regularly
The American Heart Association recommends at least 150 minutes of moderate aerobic activity per week (such as brisk walking, swimming, or cycling) or 75 minutes of vigorous activity. Even 30 minutes of walking five days a week significantly reduces cardiovascular risk. Exercise lowers blood pressure, improves cholesterol, reduces weight, and directly strengthens the heart muscle.
5. Eat a Heart-Healthy Diet
Focus your diet on:
- Vegetables and fruits — especially dark leafy greens, berries, and tomatoes
- Whole grains — oats, brown rice, whole wheat, millets
- Legumes — lentils, chickpeas, beans (rich in soluble fibre)
- Healthy fats — olive oil, avocado, nuts, seeds, fatty fish
- Reduce salt — aim for less than 2,300 mg sodium per day
- Limit processed foods, red meat, full-fat dairy, and fried foods
- Limit added sugar — sugary beverages are particularly harmful
For guidance on natural foods and herbs that support heart health, explore our Herbs & Ayurveda and Nutrition & Diet sections at HerbeeLife.
6. Stop Smoking
If you smoke, quitting is the single most impactful action you can take for your heart health. Within one year of quitting, your risk of coronary heart disease is cut by 50%. Within 15 years, your risk approaches that of someone who never smoked.
7. Maintain a Healthy Weight
Losing even 5–10% of your body weight if you are overweight can significantly improve blood pressure, cholesterol, and blood sugar. Focus on sustainable dietary changes and regular physical activity rather than crash diets.
8. Manage Stress
Chronic stress is an independent risk factor for heart disease. Evidence-based stress management techniques include regular physical activity, meditation and mindfulness, adequate sleep (7–9 hours), social connection, and where appropriate, professional psychological support. Visit our Mind & Wellbeing and Meditation & Mindfulness resources for practical guidance.
9. Know Your Family History
If first-degree relatives had heart disease, especially at a young age, inform your doctor. This may warrant earlier and more aggressive cardiovascular screening and preventive measures.
10. Get Regular Health Screenings
Many of the risk factors for heart attack — high blood pressure, high cholesterol, diabetes, and atherosclerosis — have no symptoms until they have caused significant damage. Regular health check-ups, including lipid panels, blood glucose testing, blood pressure monitoring, and ECGs after a certain age, can detect these conditions before they become crises.
Life After a Heart Attack: Recovery and What to Expect
Surviving a heart attack is not the end of the story — it is the beginning of a new and critically important chapter. The choices made in the weeks, months, and years after a heart attack have a profound effect on whether a second event occurs.
Cardiac Rehabilitation
Cardiac rehabilitation is a medically supervised programme that includes monitored exercise, education on heart-healthy living, and psychological support. Studies consistently show that patients who complete cardiac rehabilitation have significantly better long-term outcomes — lower rates of re-hospitalisation, lower mortality, and better quality of life. If your doctor recommends cardiac rehab after a heart attack, do not skip it.
Medications After a Heart Attack
Most heart attack survivors will be prescribed a combination of medications to prevent a second event, including:
- Antiplatelet agents (aspirin and/or clopidogrel) to prevent blood clots
- Beta-blockers to reduce heart rate and blood pressure
- ACE inhibitors or ARBs to protect heart function and lower blood pressure
- Statins to lower LDL cholesterol and stabilise arterial plaque
Taking these medications exactly as prescribed is one of the most important actions a heart attack survivor can take. Do not stop or adjust dosages without consulting your cardiologist.
Emotional Recovery
Depression and anxiety are extremely common after a heart attack — affecting 20–30% of survivors. These conditions are not signs of weakness; they are normal psychological responses to a life-threatening event. They are also clinically significant: untreated depression after a heart attack is associated with a significantly higher risk of a second cardiac event. Seek support — whether through your healthcare team, a mental health professional, or a cardiac support group.
▶️ Watch: Heart Attack Warning Signs — Video Guide
Want a deeper visual walkthrough of these heart attack warning signs and prevention strategies? Watch our detailed video on the HerbeeLife YouTube channel — and don’t forget to subscribe for weekly health and wellness content.
▶ Watch the Video Here 🔔 Subscribe to HerbeeLifeFrequently Asked Questions About Heart Attack Warning Signs
Conclusion: What You Do in the Next Minute Could Save a Life
Heart attack warning signs are not always dramatic. They are not always unmistakable. They are often quiet, easy to dismiss, easy to explain away with a more comfortable narrative — “it’s just stress,” “it’s probably indigestion,” “I’m probably just tired.”
The information in this article exists for one purpose: so that when your body sends you a signal, you have the knowledge to hear it correctly.
Know the warning signs. Know that they are different for women than for men. Know that silent heart attacks are real and more common than most people think. Know that the first hour after symptoms begin is the most critical window for successful treatment. And know that if you are ever in doubt — call emergency services. A false alarm is an inconvenience. A delayed response to a real heart attack is potentially fatal.
Share this article. Send it to someone you love. The life it saves might be theirs.
📖 Sources & Medical References
- American Heart Association — Warning Signs of a Heart Attack
- American Heart Association — Heart Attack Symptoms in Women
- Mayo Clinic — Heart Attack: Symptoms & Causes
- Mayo Clinic — Heart Disease in Women
- Cleveland Clinic — Silent Heart Attack
- WebMD — Heart Attack: Causes, Symptoms & Treatment
- Medical News Today — Heart Attack in Women: Symptoms & Risk Factors
- Goshen Health — Heart Attack Warning Signs & Risk Factors
- Asian Heart Institute — Silent Heart Attack: Symptoms, Causes & Prevention
- World Health Organization — Cardiovascular Diseases Fact Sheet
- American Heart Association — CPR Guidelines 2025
- Office on Women’s Health — Heart Attack Symptoms
🌿 Follow HerbeeLife for More Health & Wellness Content
Join thousands of readers on a journey to better, healthier, more natural living.
Facebook · X / Twitter · Instagram · YouTube · Pinterest