Almost everyone has experienced it — that small, round, exquisitely painful sore on the inside of the cheek, the tongue, or the soft palate that makes every sip of tea, every bite of food, and every normal swallow a minor ordeal. Mouth ulcers (oral ulcers, aphthous ulcers, or mukhpak in the Ayurvedic tradition) are among the most common conditions in the world, affecting approximately 20% of the population at any given time and an estimated 50% of people recurrently throughout their lifetimes.
Despite their near-universal familiarity, mouth ulcers are frequently mismanaged — treated with temporary topical pain relief while their underlying causes go unaddressed, leading to the cycle of recurrent episodes that many people accept as simply “something they get.” The truth is that recurrent aphthous ulcers, in most cases, have identifiable and addressable contributing factors: nutritional deficiencies, gut health disruptions, hormonal fluctuations, immune dysregulation, specific food sensitivities, and stress-driven immune suppression are among the most common and most correctable.
This guide covers the complete clinical framework for oral ulceration — the different types and their distinct management implications, the nutritional and systemic factors that drive recurrent episodes, 12 natural and evidence-supported remedies for faster healing and recurrence prevention, the Ayurvedic understanding of Mukhapaka (mouth ulcers), and the critical warning signs that distinguish common aphthous ulcers from lesions requiring urgent medical evaluation.
What Oral Ulcers Actually Are — The Tissue Biology
An oral ulcer is a full-thickness breach in the epithelium lining the oral mucosa — the soft tissue surface of the mouth. Unlike an erosion (which involves only the superficial epithelial layers), a true ulcer extends through the entire epithelial thickness into the underlying connective tissue (lamina propria), producing the characteristic appearance: a central pale-yellow or white depressed area (the exposed connective tissue, covered by a fibrinous exudate) surrounded by an erythematous (red) inflammatory halo, with the surrounding tissue raised and oedematous.
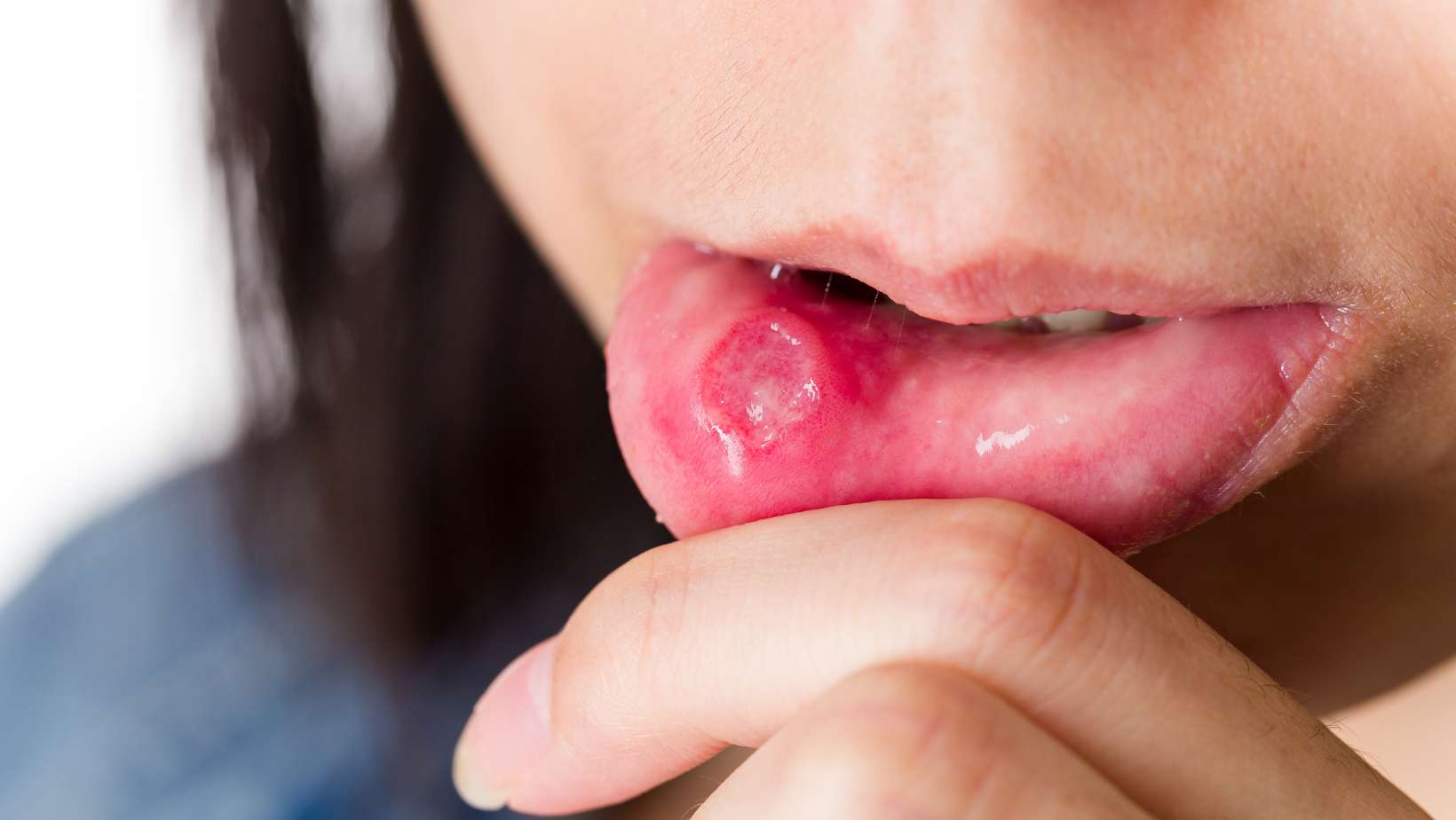
The pain of oral ulcers is disproportionate to their size because the oral mucosa is richly innervated with sensory nerve fibres — the trigeminal nerve supplies the oral cavity with one of the densest sensory innervations of any body surface. Exposed nerve fibres in the ulcer base (the connective tissue has rich peptidergic innervation) are continuously stimulated by saliva, food, temperature changes, and mechanical contact, explaining why even a 3mm ulcer can produce significant functional impairment.
Healing follows the standard wound healing sequence (haemostasis, inflammation, proliferation, remodelling) but is significantly modified by the oral environment — constant saliva exposure, continuous mechanical stimulation, and the oral microbiome’s presence at the wound site. The typical healing time for an uncomplicated minor aphthous ulcer is 7–14 days; disruption of any healing phase prolongs this timeline.
Types of Oral Ulceration — The Classification That Determines Management
Type 1: Recurrent Aphthous Stomatitis (RAS) — The Most Common Type
Recurrent aphthous stomatitis is the most prevalent form of oral ulceration — affecting approximately 20% of the general population with recurring episodes and representing the majority of mouth ulcer presentations. Despite its prevalence, the precise aetiology of RAS remains incompletely understood, and it is likely a final common pathway for multiple triggering mechanisms rather than a single disease entity.
RAS is classified into three clinical subtypes with different presentations and management implications:
Minor RAS (Mikulicz ulcers) accounts for approximately 80% of all RAS. Individual ulcers are small (less than 1cm diameter), round or oval with a well-defined yellow-white centre and erythematous halo, heal within 7–14 days without scarring, and affect non-keratinised mucosa (cheek, floor of mouth, ventral tongue, soft palate) — not the gingiva, hard palate, or dorsal tongue (which are keratinised). Episodes recur 3–6 times yearly in most affected individuals, though some experience near-continuous ulceration with new episodes appearing before current ulcers have healed.
Major RAS (Sutton’s disease) accounts for approximately 10–15% of RAS. Individual ulcers exceed 1cm and may reach several centimetres, are deeper with raised irregular margins, take weeks to months to heal, frequently scar, and can affect keratinised mucosa including the gingiva, hard palate, and dorsal tongue — atypical sites for minor RAS. Major RAS can significantly impair eating, drinking, and speaking and may require prescription treatment. The resemblance of large major RAS lesions to oral squamous cell carcinoma (see below) requires careful clinical examination and, when uncertainty exists, biopsy.
Herpetiform RAS accounts for approximately 5–10% of RAS. It presents as crops of 10–100 tiny ulcers (1–3mm) that may coalesce into larger irregular erosions. Despite its name, it has no relationship to herpes virus infection — the name reflects the clinical resemblance to herpetic gingivostomatitis. It is most common in women and older adults.
Type 2: Traumatic Oral Ulcers
Traumatic ulcers result from mechanical, thermal, or chemical injury to the oral mucosa and account for a significant proportion of oral ulcer presentations, particularly in individuals with dental appliances (braces, dentures, plates) or who habitually bite the inner cheek or tongue. Traumatic ulcers are typically: single, at an anatomically explicable location (adjacent to a sharp tooth, beneath a denture flange, at the site of repeated biting), irregular in outline rather than the regular round/oval shape of aphthous ulcers, and resolve within 10–14 days once the causative trauma is eliminated.
Chemical traumatic ulcers from aspirin placement (some individuals place aspirin tablets directly against an aching tooth, producing chemical burns) or from topical application of strong substances present as white sloughing areas with surrounding erythema. Management is elimination of the causative factor — after which healing is expected within 7–14 days. Persistence beyond 3 weeks after trauma elimination warrants professional evaluation.
Type 3: Viral Oral Ulcers — Primary Herpetic Gingivostomatitis
Primary infection with herpes simplex virus type 1 (HSV-1) in children typically presents as primary herpetic gingivostomatitis — a dramatic clinical illness with high fever (38–40°C), irritability, refusal to eat or drink (due to severe oral pain), multiple crops of small vesicles that rapidly break down into painful ulcers on both the keratinised and non-keratinised oral mucosa, generalised gingival inflammation, and regional lymphadenopathy. This presentation is clinically distinct from RAS — the involvement of keratinised mucosa (gingiva, hard palate), systemic fever and malaise, the vesicular stage before ulceration, and the first-episode character in a young child are all distinguishing features.
Recurrent intraoral herpes (in adults) typically presents as a small cluster of ulcers on keratinised mucosa (most commonly the hard palate or attached gingiva) — importantly different from the non-keratinised site predilection of RAS. Management for primary herpetic gingivostomatitis includes supportive care, adequate analgesia (critical to maintain hydration), and antiviral therapy (acyclovir) for severe cases or immunocompromised individuals.
Type 4: Oral Ulcers as a Sign of Systemic Disease
Several systemic conditions produce oral ulcers as a significant or presenting feature — making appropriate diagnosis essential before managing as simple aphthous ulcers. The most clinically important include:
Haematological deficiencies: Iron deficiency anaemia, folate deficiency, and Vitamin B12 deficiency are among the most common and most correctable causes of recurrent aphthous-pattern oral ulcers. These deficiencies impair epithelial renewal and mucosal immune function through specific mechanisms — the oral mucosal epithelium is among the most rapidly renewing tissues in the body (complete turnover every 7–14 days) and is therefore exquisitely sensitive to micronutrient deficiencies that affect DNA synthesis and cell division. Patients with recurrent oral ulcers should have full blood count, serum ferritin, folate, and Vitamin B12 levels measured before prolonged symptomatic treatment.
Inflammatory bowel disease: Both Crohn’s disease and ulcerative colitis are associated with oral ulcers — approximately 10–30% of people with Crohn’s disease have oral manifestations, including aphthous-type ulcers and specific Crohn’s-associated granulomatous lesions (cobblestoning, linear ulcers, mucosal tags). Oral ulcers may precede gastrointestinal symptoms by months or years in some patients. The gut-oral mucosal connection here is direct and mechanistically important — the same dysbiotic and inflammatory processes driving intestinal inflammation also affect the oral mucosa. The gut health framework in our guide to improving digestion naturally is directly relevant to this dimension of oral ulcer management.
Coeliac disease: Oral aphthous ulcers occur in approximately 4–10% of coeliac disease patients and may be the first presenting manifestation. The mechanism involves gluten-triggered immune activation that affects the oral mucosa alongside the intestinal mucosa — and many coeliac patients find significant improvement in oral ulcer frequency on a strict gluten-free diet even before other gastrointestinal symptoms resolve.
Behçet’s disease: A rare multi-system vasculitis characterised by the triad of recurrent oral ulcers (always present), genital ulcers, and uveitis (eye inflammation). Oral ulcers in Behçet’s are indistinguishable from aphthous ulcers clinically — the diagnosis requires the additional features. This diagnosis should be considered in patients from populations with higher Behçet’s prevalence (Middle Eastern, Eastern Mediterranean, East Asian) who have very frequent, severe recurrent oral ulcers alongside genital sores or eye symptoms.
Type 5: Oral Squamous Cell Carcinoma — The Diagnosis That Must Never Be Missed
Oral squamous cell carcinoma can present as an ulcer — typically a single, painless (or disproportionately painless for its size), irregular, indurated (hard on palpation), non-healing ulcer that has been present for more than 3 weeks without improvement. It most commonly occurs on the lateral tongue (sides), floor of the mouth, and retromolar region — sites that are also frequent for major RAS, making clinical differentiation important.
Risk factors include tobacco use in any form (smoking, bidi, gutka, paan with tobacco — all strongly associated in Indian populations), heavy alcohol consumption, prior HPV infection, and increasing age. The key clinical rule: any oral ulcer that has not healed within 3 weeks requires professional evaluation to exclude malignancy. This is the most important safety message in all oral ulcer management — and one that no amount of natural remedy should delay when an ulcer is persistent, indurated, or in a high-risk site.
The Nutritional Deficiencies Behind Recurrent Mouth Ulcers — The Most Actionable Finding
For the large proportion of people with recurrent aphthous stomatitis (RAS), identifying and correcting nutritional deficiencies is the most impactful intervention available — and one that most people managing their ulcers with topical treatments entirely miss.
A systematic review published in the Journal of Oral Pathology and Medicine found that patients with recurrent aphthous stomatitis have significantly higher rates of deficiency in: serum ferritin (iron stores), serum folate, serum Vitamin B12, and serum Vitamin D compared to matched controls without oral ulcers. A clinical study found that correcting the identified deficiency produced significant reduction in oral ulcer frequency and severity in 74% of affected patients — without any other intervention. This is one of the most practically significant findings in oral medicine: most recurrent aphthous stomatitis has a correctable nutritional basis that is identified by basic blood testing.
Iron deficiency impairs mucosal immune function and epithelial cell renewal — the oral mucosa is among the most iron-sensitive tissues due to its rapid cell turnover rate. Iron deficiency is particularly common in Indian women due to menstrual blood loss, dietary non-haem iron predominance, and the phytic acid in the predominantly grain-and-legume diet that inhibits non-haem iron absorption. The combined oral ulcer and dietary iron context connects to our article on hair fall after 30 in women — the same iron deficiency that causes hair fall also causes oral ulcers through the same mucosal renewal impairment mechanism.
Vitamin B12 deficiency impairs DNA synthesis in rapidly dividing cells — including oral mucosal epithelial cells — reducing their renewal capacity and increasing susceptibility to ulceration. B12 deficiency is endemic in Indian vegetarians, who have no dietary source of this animal-product-exclusive vitamin without supplementation or fortified foods. It is the single most important blood test to obtain in a vegetarian or vegan patient with recurrent oral ulcers.
Folate deficiency similarly impairs epithelial cell renewal (folate is required for thymidine synthesis in DNA replication) and is associated with both oral ulceration and macrocytic anaemia. Indian diets with high levels of cooking that destroys folate (extended boiling of vegetables) are common contributors.
Vitamin D deficiency — prevalent in 50–94% of the Indian urban population as covered in our immune system guide — impairs oral mucosal immune surveillance through its role in regulating the mucosal immune cells (Langerhans cells, T-regulatory cells) that maintain oral epithelial homeostasis and prevent aberrant immune activation that produces aphthous ulcers.
12 Natural Remedies for Mouth Ulcers — With Evidence and Mechanisms
1. Warm Salt Water Rinse — The First-Line Evidence-Backed Remedy
Warm salt water rinse is the most universally recommended, most evidence-supported, and most accessible natural oral ulceration remedy — and its mechanisms go well beyond simple “cleaning.” Saline solution at appropriate concentration (isotonic — similar to body fluid concentration) provides multiple therapeutic effects simultaneously: the mild osmotic action of salt draws fluid from oedematous ulcer margins, reducing the swelling that amplifies pain; the warm temperature increases local blood flow, supporting immune cell delivery and tissue repair; and the salt creates a transiently inhospitable environment for oral bacteria that colonise the ulcer base and can impede healing.
Hypertonic saline (stronger than body fluid concentration — more than a teaspoon of salt per cup of water) produces greater osmotic effects but can paradoxically irritate and damage already compromised oral mucosal tissue — the correct preparation is approximately half a teaspoon of salt per 250ml of warm water (approximately isotonic). Rinsing for 30–60 seconds 2–3 times daily (particularly after meals, when food debris colonises the ulcer) is the optimal protocol.
2. Coconut Oil — Anti-Inflammatory and Antimicrobial Oil Pulling
Coconut oil contains lauric acid — a medium-chain saturated fatty acid that is converted by salivary enzymes to monolaurin, a monoglyceride with documented antimicrobial activity against gram-positive bacteria (including Streptococcus mutans, the primary cariogenic organism), Candida species, and several viruses including HSV-1. This antimicrobial profile is directly relevant to oral ulcer management — colonisation of ulcer beds by oral bacteria prolongs the inflammatory phase of healing and delays re-epithelialisation.
Oil pulling with coconut oil — swishing 1–2 tablespoons of coconut oil in the mouth for 10–20 minutes — has traditional Indian (Ayurvedic gandhoosh) and emerging clinical support for reducing oral bacterial load. A randomised clinical trial published in the Nigerian Medical Journal found oil pulling with coconut oil significantly reduced Streptococcus mutans counts and plaque indices comparable to chlorhexidine mouthwash — the gold standard pharmaceutical oral antimicrobial. For oral ulcers specifically, applying a small amount of cold-pressed coconut oil directly to the ulcer surface several times daily reduces colonisation and provides a physical barrier against ongoing irritation.
3. Raw Honey (Particularly Manuka or Dark Honey Varieties)
Raw honey — particularly dark honey with high antimicrobial activity — is one of the most evidence-supported topical remedies for wound healing, with direct clinical evidence for oral ulcer healing specifically. A randomised controlled trial published in the Quintessence International journal found honey applied topically to recurrent aphthous ulcers significantly reduced ulcer size, healing time, pain, and recurrence compared to an over-the-counter acyclovir cream — representing genuine clinical evidence for honey’s superior performance to a pharmaceutical comparison in RAS management.
The mechanisms are multiple: the high osmolarity of honey dehydrates bacteria at the wound surface (bacteria cannot tolerate the extremely low water activity of honey); its naturally occurring hydrogen peroxide (produced by glucose oxidase from nectar glucose) provides sustained antimicrobial activity; its acidic pH (3.2–4.5) is inhospitable to most oral bacteria; and its polyphenol content (particularly methylglyoxal in Manuka honey) provides additional antimicrobial activity that is retained in the acidic wound environment. Beyond antimicrobial action, honey’s high sugar content provides the energy substrate for regenerating epithelial cells at the ulcer margin, and its anti-inflammatory flavonoid content reduces the inflammatory response that causes the pain and prevents healing progression.
Application: Apply a small amount of raw honey (dark, unheated, unprocessed varieties are most effective) directly to the ulcer surface using a clean finger or cotton swab. Allow to remain in contact for 1–2 minutes before the saliva dilutes it. Apply 4–6 times daily. The initial application may cause brief intensification of pain (the osmotic effect on exposed nerve fibres) followed by significant pain relief within 5 minutes as the nerve-calming and anti-inflammatory effects develop.
4. Triphala Mouthwash — Ayurveda’s Best-Evidenced Oral Remedy
Triphala — the classical Ayurvedic three-fruit combination (amla, haritaki, bibhitaki) — has documented antimicrobial, anti-inflammatory, astringent, and wound-healing properties that make it particularly well-suited for oral ulcer management. Triphala mouthwash (Triphala powder dissolved in warm water, strained, and used as a rinse) is one of the Ayurvedic oral care preparations with the strongest modern research evidence.
A randomised controlled trial published in the Journal of Clinical and Diagnostic Research found Triphala mouthwash as effective as chlorhexidine (the pharmaceutical gold standard for oral antimicrobials) for reducing plaque, gingivitis, and oral bacterial counts — with comparable efficacy and superior tolerability. The gallic acid, ellagic acid, and chebulinic acid in Triphala have documented anti-inflammatory effects on oral mucosal cells, reducing the NF-κB-driven inflammatory response that prolongs the painful phase of ulcer healing. Amla’s Vitamin C content (the richest stable natural source available) directly supports collagen synthesis for re-epithelialisation — the structural protein that fills the ulcer defect during healing.
Preparation: Dissolve half a teaspoon of Triphala powder in 200ml of warm water. Allow to steep for 5 minutes. Strain through a fine cloth or tea strainer (the undissolved powder particles can irritate ulcers). Use as a mouthwash for 30–60 seconds, 2–3 times daily. The taste is strongly astringent — this is the tannin content producing the mouth-drying and tissue-tightening effect that supports ulcer healing.
5. Turmeric Paste — Anti-Inflammatory and Antimicrobial Direct Application
Turmeric’s curcumin has documented anti-inflammatory activity through NF-κB inhibition, prostaglandin synthesis reduction, and free radical scavenging — mechanisms directly relevant to the inflammatory phase of oral ulcer pathogenesis and healing. A clinical study published in the Journal of Indian Society of Periodontology found that topical application of 2% curcumin gel to recurrent aphthous ulcers significantly reduced ulcer size, pain, and healing time compared to placebo gel.
The antimicrobial dimension of turmeric is also relevant — curcumin has documented activity against Streptococcus mutans and several other oral bacteria, reducing the bacterial colonisation that delays ulcer healing. The bioavailability concern that limits curcumin’s systemic effects (fat and piperine required for absorption) is less relevant for topical application — direct tissue contact delivers curcumin to the ulcer surface regardless of systemic absorption.
Preparation: Mix a small pinch of turmeric powder with enough raw honey (or coconut oil) to form a thick paste. Apply directly to the ulcer using a clean finger. Allow to remain for 2–3 minutes before rinsing. The combination of turmeric’s anti-inflammatory and antimicrobial effects with honey’s wound-healing properties creates a synergistic topical preparation. Caution: turmeric stains yellow — avoid before any activity where yellow-stained lips or surrounding tissue would be conspicuous.
6. Aloe Vera Gel — The Wound-Healing and Anti-Inflammatory Succulent
Aloe vera gel has documented wound-healing properties through multiple mechanisms relevant to oral ulcer healing: it contains acemannan (a polysaccharide that activates macrophages, stimulates collagen synthesis, and promotes epithelial cell proliferation — all critical for the proliferative phase of wound healing), aloesin (a chromone compound with anti-inflammatory effects comparable to hydrocortisone in some assays), and a cooling, demulcent quality that provides immediate pain relief through the same sensory competition mechanism as menthol.
A randomised clinical trial published in Dental Research Journal found that aloe vera gel applied topically to recurrent aphthous ulcers significantly reduced pain and healing time compared to an over-the-counter benzocaine gel (a common pharmacological topical anaesthetic) — providing clinical evidence that aloe vera is not merely comforting but genuinely superior to standard OTC treatments in this application. The gel forms a physical barrier over the ulcer that protects exposed nerve endings from salivary and food contact, producing sustained pain reduction between applications.
Application: Apply fresh aloe vera gel (extracted from a leaf of a home plant, if available — commercial gels should be pure without additives) directly to the ulcer using a clean swab. Apply 3–4 times daily. Fresh gel is more bioactive than commercial preparations — the acemannan degrades relatively quickly after extraction.
7. Liquorice Root (Mulethi) — The Inflammation and Stress Dual Remedy
Liquorice root (Glycyrrhiza glabra) — known as mulethi in Hindi — has specific evidence for recurrent aphthous stomatitis that makes it one of the most targeted Ayurvedic remedies for this condition. A randomised controlled trial published in Oral Diseases found that liquorice root extract mouthwash significantly reduced the pain, size, and healing time of recurrent aphthous ulcers compared to placebo — with the effect attributed to glycyrrhizin (the primary bioactive compound) and its anti-inflammatory and wound-healing properties.
The mechanisms include: glycyrrhizin’s direct anti-inflammatory activity through inhibition of 11β-hydroxysteroid dehydrogenase (producing a mild local cortisol-mimetic effect at the ulcer site without systemic steroid exposure); liquorice’s documented adaptogenic effects that reduce HPA axis reactivity (stress — one of the most common RAS triggers — operates through cortisol-driven immune dysregulation that mulethi addresses at its hormonal source); and the demulcent quality of liquorice root that creates a protective coating over oral mucosal surfaces. The comprehensive adaptogenic profile of liquorice is related to the stress management approaches in our ashwagandha for stress and anxiety guide — both herbs addressing the HPA axis dysregulation that drives stress-triggered oral ulcers.
Preparation: Steep 1 teaspoon of dried mulethi pieces (or mulethi powder) in 250ml of boiling water for 10 minutes. Allow to cool to warm. Use as a mouthwash, swishing for 30–60 seconds, 2–3 times daily. Alternatively, chewing a small piece of dried mulethi root directly provides sustained local delivery of glycyrrhizin to the oral mucosa.
8. Vitamin B12 Supplementation — Often the Most Important Internal Remedy
Based on the evidence above regarding nutritional deficiencies, Vitamin B12 supplementation deserves specific mention as one of the highest-impact internal interventions for recurrent oral ulcers in Indian populations — particularly for vegetarians and vegans who have no dietary source of this vitamin.
A randomised controlled trial published in the Journal of the American Board of Family Medicine found that Vitamin B12 supplementation (1,000mcg sublingually daily) significantly reduced RAS frequency, duration, and pain intensity compared to placebo over 6 months — with 74% of participants in the B12 group achieving “no aphthous ulcers” in the final month of the study versus 32% in the placebo group. This is one of the most dramatic treatment response rates published for any RAS intervention, reflecting the fundamental role of B12 in mucosal epithelial renewal.
Sublingual B12 (methylcobalamin — the most bioavailable and most neurologically relevant form) bypasses the intrinsic factor-dependent absorption mechanism in the small intestine that is often impaired in both dietary deficiency and age-related gastric atrophy, making it effective even in people whose oral B12 supplementation has not previously resolved their deficiency.
9. Clove Oil — The Natural Oral Anaesthetic
Clove oil (containing eugenol as its primary active compound) is one of the most potent natural oral anaesthetics available — eugenol directly blocks sodium channels in pain-conducting nerve fibres (a mechanism shared with topical anaesthetics like benzocaine and lidocaine) and also inhibits prostaglandin synthesis, providing both anaesthetic and anti-inflammatory effects. It is used as a dental anaesthetic by professionals globally and has documented efficacy for oral pain management.
For oral ulcer pain relief specifically, a small amount of diluted clove oil (one drop of clove essential oil in a teaspoon of coconut or sesame oil) applied directly to the ulcer using a cotton swab provides rapid pain relief lasting 20–30 minutes — comparable to commercial topical anaesthetic preparations. Undiluted clove essential oil is too concentrated for direct oral mucosal application and can cause chemical burns — always dilute with a carrier oil. The combined eugenol content of clove oil and the lauric acid antimicrobial effect of coconut oil as carrier creates a dual anaesthetic-antimicrobial preparation for symptomatic management.
10. Stress Management — Addressing the Most Common RAS Trigger
Stress is one of the most consistently reported triggers for recurrent aphthous stomatitis — with studies showing that 50–60% of RAS patients identify psychological stress as a preceding trigger for new ulcer episodes. The mechanism is immunological: cortisol released during stress suppresses mucosal immune surveillance (particularly IgA secretory antibody production, the primary immunoglobulin protecting oral and gastrointestinal mucosal surfaces) and shifts mucosal immunity toward an aberrant Th1-mediated response that produces the tissue-damaging cytokine environment of aphthous ulcer formation.
Managing the stress-ulcer relationship requires both acute intervention (preventing the cortisol-mediated immune dysregulation during acute stressors) and chronic resilience building (raising the HPA axis threshold that determines whether stress produces immune dysregulation severe enough to trigger ulcers). The comprehensive stress management and cortisol regulation frameworks in our yoga for stress relief guide, power of meditation guide, and ashwagandha for stress and anxiety guide collectively address this stress-immune dysregulation pathway at multiple levels.
11. Probiotic Supplementation — Supporting Oral and Gut Mucosal Immunity
The emerging role of the oral microbiome in aphthous ulcer pathogenesis — with RAS patients showing altered oral microbial communities compared to ulcer-free controls — makes probiotic support a rational intervention for recurrent oral ulcers. Lactobacillus rhamnosus GG and Lactobacillus acidophilus supplementation have shown the most promising preliminary evidence for reducing RAS frequency, with the proposed mechanisms including restoration of the oral microbiome balance that competes with pathogenic bacteria colonising ulcer sites and modulation of oral mucosal immune function toward regulatory rather than inflammatory T-cell responses.
Beyond the direct oral microbiome effect, the gut-oral mucosal immune axis — the same microbiome-immunity connection discussed in our digestion guide — is clinically relevant here: the gut microbiome produces sIgA antibodies that are distributed to all mucosal surfaces, including the oral mucosa. Improving gut microbiome health through the dietary and fermented food strategies covered in our digestion guide therefore supports oral mucosal immunity through this systemic mucosal immune axis.
12. Dietary Trigger Identification and Avoidance
Several specific food substances act as direct triggers for recurrent aphthous ulcers through both immune-mediated and mechanical mechanisms. The most consistently identified include:
Sodium lauryl sulphate (SLS) — a foaming agent present in most commercial toothpastes and mouthwashes — is the most consistently documented dietary/product trigger for RAS, with multiple studies showing significant reduction in ulcer frequency in SLS-sensitive individuals who switch to SLS-free toothpaste. SLS disrupts the mucosal protective glycoprotein layer of the oral epithelium, increasing permeability and susceptibility to ulcer formation. Switching to an SLS-free toothpaste (available in Indian pharmacies and health stores) is a simple, cost-effective intervention that produces dramatic improvement in SLS-sensitive individuals (estimated 15–30% of RAS patients).
Acidic foods and beverages: Citrus fruits, tomatoes, pineapple, and vinegar-based foods can trigger ulcer formation in susceptible individuals through direct mucosal acidification, particularly on already compromised mucosa. Identifying and temporarily reducing these foods during active ulcer episodes accelerates healing by reducing the pH challenge to the repairing epithelium.
Gluten: As discussed above, coeliac disease and non-coeliac gluten sensitivity both produce oral ulcers — and a gluten-free trial for 3 months is a reasonable investigation in individuals with frequent severe RAS unresponsive to other interventions, particularly if accompanied by any digestive symptoms.
The Ayurvedic Understanding of Mukhapaka — Mouth Ulcers as Pitta Excess
Ayurveda classifies mouth ulcers (Mukhapaka — literally “cooking of the mouth”) as a predominantly Pitta condition — reflecting the fire, heat, inflammation, and burning quality of the condition with characteristic Pitta excess symptoms. The treatment approach in classical Ayurveda is systematically Pitta-pacifying: cooling herbs (mulethi, neem, coriander, fennel), cooling foods (coconut, pomegranate, coriander water), avoiding Pitta-aggravating triggers (excess spicy food, sour foods in excess, alcohol, heat exposure), and the internal cleansing that addresses the systemic Pitta accumulation driving the oral manifestation.
Gandoosha (oil pulling) and Kavala Dharana (medicated mouthwash retention) are the primary Ayurvedic oral therapeutic procedures for Mukhapaka — both involving retained contact between therapeutic substances and the oral mucosa for extended periods, maximising tissue penetration and therapeutic effect duration. These are the practical predecessors of modern oral drug delivery systems — and the clinical evidence accumulating for oil pulling (discussed above) validates the pharmacological rationale of this ancient practice.
The Ayurvedic dietary guidance for Mukhapaka specifically includes: avoiding tamarind (amla sour foods), excess citrus, tobacco, alcohol, and very spicy foods during episodes; consuming coriander water, coconut water, pomegranate juice, and cooling dairy preparations (buttermilk, plain curd); and using Triphala as both internal medicine and external mouthwash to address the digestive imbalance that Ayurveda identifies as the root cause of recurrent oral inflammation. This digestive root-cause perspective aligns with the contemporary evidence on gut microbiome, inflammatory bowel disease, and coeliac disease as systemic drivers of oral ulceration.
Oral Ulceration: Myth vs. Fact
| ❌ The Myth | ✅ The Truth |
|---|---|
| Mouth ulcers are caused by eating too much spicy or hot food | Spicy and acidic foods can aggravate existing ulcers (prolonging pain and healing time) and can trigger episodes in susceptible individuals — but they are not the primary cause of recurrent aphthous stomatitis. The primary causes are nutritional deficiencies (B12, iron, folate, Vitamin D), stress-driven immune dysregulation, hormonal fluctuations, gut health disruption, and specific product sensitivities (particularly SLS in toothpaste). Dietary modification is supportive but rarely sufficient without addressing these underlying factors. |
| Mouth ulcers are contagious | Recurrent aphthous stomatitis (the most common form) is not contagious — it is an immune-mediated condition that cannot be transmitted through contact, kissing, shared utensils, or any other route. Primary herpetic gingivostomatitis (caused by HSV-1) is contagious during the active ulcerative phase — this is the clinically distinct childhood illness with fever and multiple ulcers, not the typical adult recurrent aphthous pattern. |
| All mouth ulcers heal on their own — no treatment is necessary | Minor aphthous ulcers do heal spontaneously within 7–14 days — but treatment significantly accelerates healing, reduces pain, and improves quality of life during the episode. More importantly, any mouth ulcer persisting beyond 3 weeks requires professional evaluation to exclude oral squamous cell carcinoma. And recurrent ulcers that are managed symptomatically without identifying and addressing their underlying causes will continue to recur indefinitely. |
| Avoiding all acidic and spicy foods will prevent mouth ulcers | Dietary restriction beyond eliminating identified personal triggers is unnecessary and counterproductive. Many nutritious foods (citrus, tomatoes, fermented foods) are falsely restricted in the belief they cause ulcers — when the primary causes are nutritional deficiencies, stress, and systemic factors that dietary restriction without nutritional replacement worsens rather than improves. A comprehensive nutritional approach (identifying and correcting deficiencies, maintaining diverse whole food intake) is more effective than blanket dietary restriction. |
| Mouth ulcers indicate poor oral hygiene | Oral hygiene is not the primary cause or driver of recurrent aphthous stomatitis. However, poor oral hygiene does increase the bacterial colonisation of ulcer beds that prolongs the inflammatory healing phase — so adequate but gentle oral hygiene (switching to SLS-free toothpaste, using warm saline rinses after meals) is supportive of faster healing without being the root cause. |
| If you get frequent mouth ulcers, it must be due to stress alone | Stress is a significant trigger for 50–60% of RAS patients — but it is rarely the only factor. Blood tests for B12, iron (serum ferritin), folate, and Vitamin D identify correctable deficiencies in the majority of people with frequent RAS. Treating stress without investigating and correcting nutritional deficiencies produces only partial improvement in most recurrent cases. |
When to See a Doctor — Red Flags for Oral Ulcers
See a doctor or dentist promptly for any of the following: any oral ulcer persisting beyond 3 weeks without healing (oral cancer must be excluded — this is the most important rule in all mouth ulcer management); an ulcer that is painless or disproportionately painless for its size (malignant ulcers are often less painful than aphthous ulcers because they destroy nerve fibres); an ulcer with hard, raised, or everted (turned outward) edges that feel firm on gentle palpation; an ulcer associated with a palpable lymph node in the neck; multiple ulcers in a new patient who has not had prior recurrent episodes (to rule out systemic disease, drug reactions, or viral causes); ulcers in a child with fever, systemic illness, and widespread oral involvement (herpetic gingivostomatitis requires specific management); ulcers accompanied by genital ulcers or eye inflammation (Behçet’s disease consideration); and any ulcer in a person with significant tobacco or alcohol use history.
Related Articles From HerbeeLife
📖 How to Improve Digestion Naturally: 12 Powerful Science-Backed Strategies
📖 Amla Benefits: Proven Immunity, Digestion and Whole-Body Health Backed by Science
📖 Anti-Inflammatory Foods: 12 Powerful Choices That Fight Disease From the Inside Out
📖 Natural Ways to Boost Your Immune System: 12 Science-Backed Strategies
📖 Ashwagandha for Stress and Anxiety: What Actually Happens in Your Body
📖 How Hormones Affect Your Health: The Complete Guide Women Must Read
📖 Essential Herbs for Health: 10 Powerful Natural Remedies That Actually Work
Frequently Asked Questions: Mouth Ulcers (Oral Ulceration)
What is the fastest way to heal a mouth ulcer naturally?
The fastest healing combination involves: raw honey applied directly to the ulcer 4–6 times daily (clinical trial evidence for superior healing time versus pharmaceutical comparison), warm saline rinse after every meal, diluted clove oil for acute pain relief, and avoiding SLS-containing toothpaste during the episode. These interventions together typically reduce healing time from the standard 7–14 days to 4–7 days for minor ulcers. Addressing underlying nutritional deficiencies (B12, iron, folate) produces the most significant long-term improvement in both healing time and recurrence frequency.
Why do I keep getting mouth ulcers even though I eat well?
The most common reasons for frequent recurrence despite seemingly healthy eating: Vitamin B12 deficiency (nearly universal in strict vegetarians who don’t supplement — B12 is found only in animal products); iron deficiency anaemia or low ferritin (common in women with heavy menstrual periods, even with iron-containing foods — non-haem iron from plant sources is poorly absorbed); SLS sensitivity from standard toothpaste; unrecognised stress-triggered immune dysregulation; subclinical coeliac disease or gluten sensitivity; or hormonal fluctuations (particularly perimenstrual drops in oestrogen and progesterone that affect oral mucosal immunity). A comprehensive blood panel (FBC, serum ferritin, serum B12, folate, Vitamin D, and coeliac antibodies) is the most important investigation for frequent recurrent ulcers.
Is there a link between mouth ulcers and gut health?
Yes — directly and through multiple mechanisms. Inflammatory bowel disease (Crohn’s and UC) has oral manifestations in 10–30% of patients. Coeliac disease produces oral ulcers in 4–10% of affected individuals. The gut microbiome’s influence on systemic mucosal immunity (producing secretory IgA that protects all mucosal surfaces including the oral mucosa) means that gut dysbiosis directly impairs oral mucosal immune function. And the nutritional deficiencies that drive most recurrent aphthous stomatitis (B12, iron, folate) are frequently caused by impaired gut absorption rather than inadequate dietary intake. Addressing gut health through the strategies in our digestion guide is therefore a direct oral health intervention.
Is oil pulling with coconut oil effective for mouth ulcers?
Oil pulling has clinical evidence for reducing oral bacterial load comparably to chlorhexidine mouthwash — which addresses the bacterial colonisation that prolongs ulcer healing. It is not a primary treatment for aphthous ulcers but is a valuable adjunct that supports healing by reducing the bacterial burden at the wound site. The optimal approach is oil pulling in the morning (before food or water) combined with warm saline rinsing after meals and direct topical application of honey or aloe vera to the ulcer surface throughout the day.
Can hormonal changes cause mouth ulcers?
Yes — the perimenstrual phase (the week before menstruation) is one of the most frequently reported RAS triggers in women, with the declining oestrogen and progesterone of the late luteal phase producing both direct effects on oral mucosal immune function (oestrogen has mucosal immunomodulatory effects through oestrogen receptor expression on oral epithelial cells) and indirect effects through the cortisol dysregulation and immune suppression that accompany premenstrual stress. Some women have a clear cyclical pattern of oral ulcers appearing 1–3 days before menstruation — identification of this pattern allows proactive intervention with B12 supplementation, stress management, and dietary support in the week preceding expected onset.
Sources and References
1. Jurge S et al. Recurrent aphthous stomatitis. Oral Diseases, 2006.
2. Altenburg A et al. Recurrent aphthous stomatitis: current concepts. JDDG, 2014.
3. Nolan A et al. Recurrent aphthous ulceration: vitamin B1, B2 and B6 status and response to replacement therapy. Journal of Oral Pathology and Medicine, 1991.
4. Volkov I et al. Effectiveness of vitamin B12 in treating recurrent aphthous stomatitis: a randomized, double-blind, placebo-controlled trial. Journal of the American Board of Family Medicine, 2009.
5. English HK et al. The effects of Manuka honey on plaque and gingivitis: a pilot study. Journal of International Academy of Periodontology, 2004.
6. Shanbhag VK. Oil pulling for maintaining oral hygiene — a review. Journal of Traditional and Complementary Medicine, 2017.
7. Gupta D, Bhaskar DJ et al. A comparison of the clinical effectiveness of Triphala and chlorhexidine mouthwash. Journal of Clinical and Diagnostic Research, 2014.
Follow HerbeeLife
🌿 Stay connected for more evidence-based oral health, Ayurvedic wisdom, and natural wellness content:
📸 Instagram | 📌 Pinterest | 👥 Facebook | 🐦 X (Twitter)
Final Thoughts: Recurring Mouth Ulcers Are Not Just Bad Luck — They Are a Message Worth Listening To
The most important thing most people with recurrent mouth ulcers need to hear is this: your body is trying to tell you something. Not something dramatic or frightening — in most cases, something as correctable as a B12 deficiency, an iron level that has quietly dropped, a stress accumulation that has crossed a threshold, or a toothpaste ingredient that has always been irritating your oral mucosa without your awareness.
Treating mouth ulcers with topical pain relief while ignoring these signals will produce the same cycle of recurrence indefinitely. Investigating and addressing the signals — with a blood test, a toothpaste change, a stress management practice, a probiotic — breaks the cycle.
Your mouth is not a separate system from the rest of your body. When it keeps breaking down in the same way, it is connected to something elsewhere in your physiology. Finding and addressing that connection is both the most effective and the most respectful response to your body’s communication.
⚠️ Medical Disclaimer: This article is for informational and educational purposes only and does not constitute medical advice. Any oral ulcer persisting beyond 3 weeks must be evaluated by a qualified dental or medical professional to exclude oral cancer. Do not delay professional evaluation because of natural remedies. Read full disclaimer →
💬 Which of these 12 natural remedies have you tried — and what triggered your breakthrough in managing recurrent mouth ulcers? Was it a nutritional deficiency you discovered? A toothpaste change? Share in the comments. This community’s collective experience is invaluable for people in the early stages of understanding their recurrent ulcers.